You are here
Part two: AHP Preceptorship
The NHS Long Term Workforce Plan published in 2023, acknowledges the importance of a comprehensive programme of support for AHPs, and preceptorship is one component of this.
Well-constructed and delivered preceptorship support can build the confidence of individual professionals as they transition into the AHP workforce for the first time. This helps them to establish their scope of professional practice as registrants and continue their professional development.
Preceptorship can also provide wrap-around support for AHPs at other points of transition within their professional careers, such as:
- Return to practice after a lengthy period away, for example from a career break.
- Join the UK workforce as an internationally educated or recruited worker.
- Change their work setting or sector.
- Return to a role after a break, for example from maternity or carers leave.
Organisations which provide AHPs with preceptorship demonstrate a commitment to an employee’s wellbeing and professional development. This benefits recruitment and retention within organisations.
The HCPC Year in registration survey 2022 identified that:
- 32% of respondents reported that they did not have a structured period of learning on entering the workplace.
- 24% reported that the period of structured support they received lasted less than three months.
Professional networks and employers working together across systems have the capacity to drive up excellence in the provision of preceptorship. This will improve early experience in role and support the aim to retain AHPs within the NHS after the first year (currently 11% AHPs leave the NHS in their first year - Electronic Staff Record (2023) – NHSE analysis).
A baseline data collection activity by the AHP Preceptorship and Foundation Support programme in 2023 found that there is variation in the AHP Preceptorship landscape. From the 172 organisational responses across NHS, social care and private, independent, or voluntary settings:
- 64% of organisations offer all their AHPs preceptorship.
- 24% of organisations offer to some of their AHPs
- 12% of organisations do not offer preceptorship to AHPs.
- 57% of organisations reported offering a multi-professional preceptorship programme.
What is unique about AHP Preceptorship?
Preceptorship is a workforce intervention that can benefit all health care professionals. The Nursing and Midwifery Council published their Principles for Preceptorship in 2022 with the national nursing preceptorship framework produced in October 2022 and the national midwifery preceptorship framework produced in March 2023. The three preceptorship frameworks are relatable to one another, however there are specific elements which mean that preceptorship for AHPs has unique considerations. These are:
- The role of the different professional development frameworks produced by Professional Bodies. These support the shaping of AHP’s careers and therefore considered in the development of content for AHP preceptorship programmes.
- The building of AHPs’ professional identity and belonging. This needs to be integrated within multi-professional preceptorship. This may be challenging to achieve for some of the small and vital professions of the AHP workforce within an organisation.
- The difficulty for AHPs from small and vital professions or those who work more independently to access same-profession support. Assistance will be required to access that support across the Integrated Care System (ICS).
- The variation in access to in-time supervision and support for the different AHPs. This is due to differences in ways of working and employment.
- The variation in the number of individuals within the different AHP groups. Local, system and regional infrastructure will need to support preceptorship for smaller professional groups.
- The different expectations about preceptorship and on-going career development across AHPs.
These unique considerations form the basis for organisation and systems working collaboratively to deliver successful AHP Preceptorship. Partnership collaboration will ensure preceptees have access to both uni-professional and multi-professional preceptorship, regardless of their professional background or their employing organisation. This also provides opportunities for the identification and scaling-up of good practice in AHP Preceptorship across different organisations.
Organisations and Systems
The AHP Preceptorship Standards and Framework acknowledges that successful implementation requires the commitment of individual organisations, including AHP leadership, and the systems which they are part of.
A system should be considered as an ICS. The ICS comprises of a network of organisations, working together in a geographically defined area, to plan and deliver integrated health and care services.
AHP leadership is a key enabler for AHP Preceptorship at an organisation and system level. This leadership includes accountability and assurance that preceptorship support is integrated within areas of work including workforce planning, professional practice, education, and human resources. Chief AHP roles within organisations and at a system level ensure a culture of continuous improvement is built around AHP Preceptorship and facilitate collaboration to achieve access and equity of preceptorship offer.
The NHS Long Term Workforce Plan reinforces the role of ICSs in creating an integrated architecture for workforce development and innovation. It is expected that each ICS will support the development of context-specific workforce plans that recruit and retain AHPs. ICSs are therefore in a key position to facilitate collaboration and partnership working that support the implementation of AHP Preceptorship.
Moreover, ICSs are well-placed to develop an architecture of professional networks and other resources that ensure that access to AHP Preceptorship is comprehensive. AHPs working in smaller health organisations, independently, across health and social care, or even in other public service areas such as education, will require opportunities outside of their employing organisations to access an appropriate mix of uni-professional and multi-professional development opportunities within their preceptorship.
Approaches to AHP Preceptorship
AHP Preceptorship programmes and their implementation should be: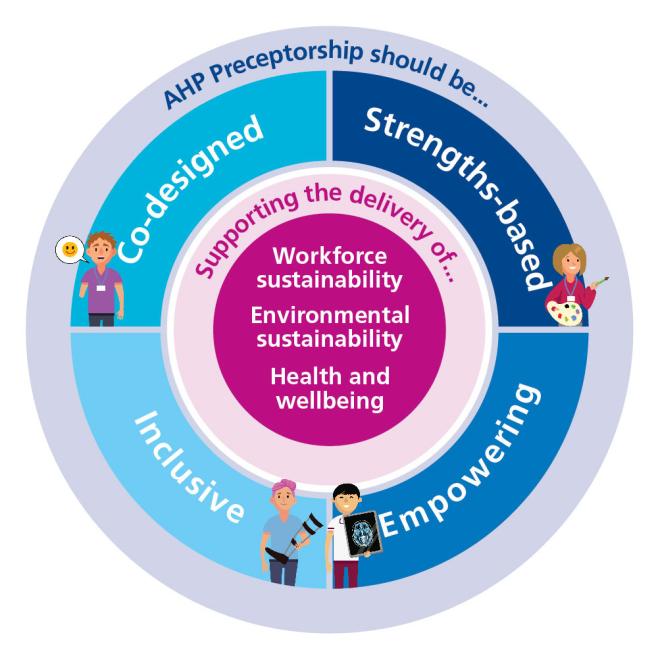
- Strengths-based – AHP Preceptorship should be a personalised experience which enables individual AHPs to achieve their potential as they transition within the workforce. Based on a needs assessment, building on previous learning experiences, and personal and professional strengths ensures that preceptorship is tailored to the individual rather than a one-size fits all approach.
- Co-designed – The implementation, review, and continuous improvement of AHP Preceptorship should be a collaborative process. This brings together the insights of different stakeholders, including individual AHPs with experiences of different career transitions. In this way, programmes will achieve greater implementability within the context of local systems and ways of working.
- Empowering – The implementation of AHP Preceptorship should empower individual AHPs to engage in their own development. This is different from workforce interventions such as induction and performance management.
- Inclusive – AHP Preceptorship should be inclusive in design and implementation. This ensures that all AHPs that could benefit from preceptorship are able to do so. At a programme level, this may require embedding preceptorship within human resources processes, including recruitment. At an individual level, this means that preceptors are familiar with differences in learning and development needs, and how these can be addressed through different styles of engagement.
AHP Preceptorship should support delivery of the following strategic aims:
- Workforce sustainability – AHP Preceptorship can contribute to a sustainable workforce by encouraging and supporting employee wellbeing and retention in organisations and professions.
- Environmental sustainability – The design of AHP Preceptorship should reflect principles of environmental sustainability, using, for example, digital solutions that facilitate record-keeping and professional networking.
- Health and wellbeing – AHP Preceptorship has the potential to achieve a wide range of outcomes important to workforce systems, organisations, and professions. At the heart of these outcomes should be the professional, career, and personal impacts of preceptorship for both preceptee and preceptor. These include their own health and wellbeing in the workplace, and practical mechanisms which protect a positive work-life balance.
Our regional networking events were an excellent opportunity to meet up and share our experiences of our own preceptorship programmes. There's definitely more sharing of good practice now.
Trust AHP Preceptorship Lead
The AHP faculty lead was able to put me in touch with dietetic service leads from other Trusts. We have been able to form a network to support us as new graduates as we settle in to the NHS
Recently Registered Dietitian