You are here
Primary care rotation
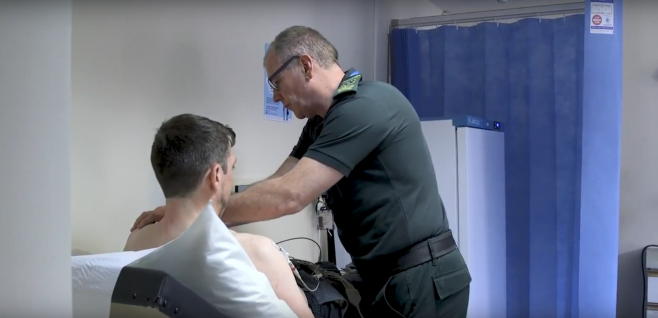
The specialist and advanced paramedics on rotation within primary care, work with one or more GP practices contributing to planned activities within the practices.
This could involve 'same day’ home visits for patients who cannot attend the surgery; seeing and treating urgent or emergency patients; concentrating on care home activity; and running clinics for selected patient groups.
This results in:
- improved responses to urgent and same day requests
- extra generalist within primary care to support GP practice workload
- improved integrated working with the ambulance service
- raising the profile of all professions as a result of integrated working.
Paramedics working within GP surgeries are supporting the practice teams to provide a responsive home visiting service as can be shown by this case from the Derbyshire pilot.
Tracy, a specialist paramedic working within a GP practice, recently attended a patient, who had contacted the practice in some distress with back pain just before 9am to request an urgent home visit.
The practice triaged the call and, realising the urgency, requested the rotating paramedic attend within the next two hours - a lot earlier than would have been possible by a GP home visit . Tracy visited the patient at home where she reviewed and changed the patient’s medication and arranged occupational therapy equipment to provide additional support. The patient remained at home and, not only was their immediate pain managed, but the occupational therapist was able to offer their expertise to promote recovery and relapse occurring again; all within their own home.
Afterwards, the patient said: “I am very happy. Tracy was very good and helped get me sorted.” The surgery agreed commenting “The paramedic rotation gives the practice access to another clinician with expert knowledge in the community, allowing us to continue working with pre-booked patients without interruption, but still with us knowing that the patient at home is being looked after.”
Specialist paramedics working within GP practices are supporting practice teams provide a responsive home visiting service as can be seen from this recent case from the Derbyshire pilot.
An elderly lady contacted the surgery after experiencing chest pain that had spread to her neck and both arms – concerning symptoms for any medical professional. The patient had a fear of being admitted to hospital and refused an ambulance. and was known to the practice and community due to her complex medical history.
The specialist paramedic attended to the patient at home and carried out an ECG and other investigations. Fortunately, these showed no life-threatening signs and the ECG was normal for the patient after being able to compare it with previous notes.
This avoiding extra anxiety for the patient, gave the practice assurance that their patient was treated to the best of their ability, in line with her wishes and beliefs.
The community matron – who knew the patient and was aware of her anxiety – was extremely happy with the service provided, explaining it was a great comfort for the patient to be cared for and reviewed in her own home and not be taken to hospital. This wouldn’t have been the case if the specialist paramedic pilot scheme had not been up and running.
Developing trusted relationships with GPs and enhanced confidence of specialist paramedics is reaping benefits for patients, as can be seen in this case study from the Lincolnshire pilot.
Having received a call from Karen, the rotating paramedic at the Emergency Operations Centre (EOC) about a patient who was experiencing breathing difficulties, Gary, a specialist paramedic visited the patient at home.
The gentleman who suffered with motor neurone disease was having difficulty in breathing. The gentleman was under expert care at the Motor Neurone Centre and he had attended a few days earlier for an examination. Gary contacted Karen back at the EOC to request information from the Centre regarding the patient’s condition on the day they had attended. The patient and their partner were desperate not to attend hospital if it could be helped.
Karen arranged a call between the consultant who had seen the patient and Gary. Armed with this vital information, Gary called the patient’s GP and presented his clinical findings together with the consultant’s information. The GP arranged a district nurse to visit to give some medication and arranged to visit the patient after surgery. When Gary gave this as an option to the patient and their family, he recalls “you could see the stress drain from the patient’s partner’s face as they felt something was being done and hospital would not be necessary” said Gary.
“On reflection, I felt as part of the health team, thanks to the way the professionals interfaced the patient was the main focus on this case and we managed an outcome all were happy with. I felt empowered and it confirmed to me what we have all being thinking, that with joint working we can change patients’ outcome for the better.”