You are here
Maternity
Contents
HEE is leading on a programme of work to help shape the future maternity workforce, supporting the vision set out in the report of the National Maternity Review, Better Births, to improve maternity care in England. We are also undertaking work in response to the recommendations of the final report of the Ockenden review of maternity services at the Shrewsbury and Telford Hospital NHS Trust.
Our Ockenden Immediate and Essential Actions catalogue provides a central location for resources to support maternity services to deliver the Ockenden recommendations and support the health and wellbeing of staff. It includes links to e-learning, toolkits and publications.
HEE is also supporting neonatal services with the implementation of the Neonatal Critical Care to help deliver the government’s ambition to reduce the rate of stillbirths, neonatal and maternal deaths and intrapartum brain injuries in babies in England by 50% by 2025, to ensure England is one of the safest places in the world to have a baby.
General enquiries: maternityprogramme@hee.nhs.uk
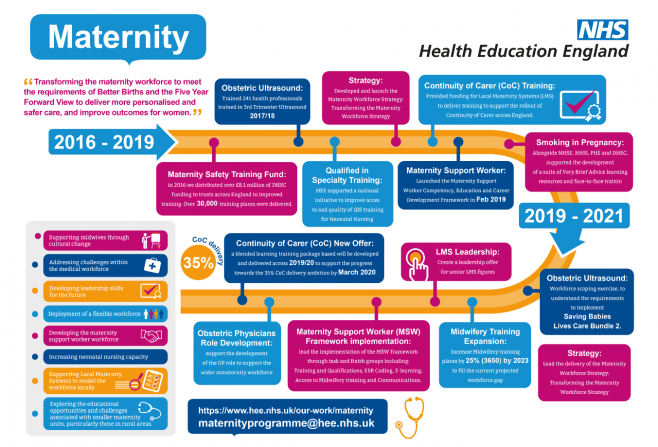
Take a look at our journey so far:
More about our maternity work:
In 2016, HEE distributed over £8.1 million of Department of Health Funding to 136 NHS Trusts across England to deliver training to improve maternity safety across a variety of key areas. All trusts provided funding committed to key actions to improve safety including developing maternity safety improvement plans and appointing maternity safety champions.
As a result of the MSTF, over 30,000 training places were delivered across multi-professional teams in England.
An independent evaluation commissioned by HEE and carried out by the University of Cumbria to assess the impacts and outcomes of training has been produced and findings will be presented at a sharing and learning event in February.
The evaluation found that maternity safety training has impacted on everyday practice through: increasing confidence and empowering the maternity staff; enhancing skills, knowledge and awareness; improving multi-professional working and communication; improving patient safety; and encouraging cultural change.
Access the independent evaluation of the fund.
HEE has continued to support maternity safety, including the development of a Saving Babies’ Lives e-Learning package on e-LfH.
The HEE Maternity Programme e-LfH Guide is designed to provide an overview of all of the e-learning packages that are related to Maternity and Pregnancy. There are a broad range of programmes, modules and individual courses available. View the HEE Maternity Programme e-LfH Guide.
For an overview of all the e-learning packages that are related to Children and Young People please download our CYP Programme e-LfH Guide.
The e-LfH platform also has a ‘Maternity and Newborn´ platform. Access the Maternity and Newborn programme here.
Maternity support workers (MSWs) are an integral part of the maternity workforce and play an important role in supporting midwives and the wider maternity teams, mothers and their babies through pregnancy, labour and during the postnatal period. However, within the current workforce, the roles, responsibilities and job titles of MSWs in England vary widely. Take a look at our work around the role of the Maternity support worker.
As part of Supported Return to Training, Health Education England (HEE) provided a grant to the Royal College of Obstetrics & Gynaecology (RCOG) to create a Return to Work Toolkit.
This is aimed at supporting O&G doctors, and their supervisors, who are returning to clinical practice and to promote a supportive and high quality learning environment.
HEE in 2019 has worked with partners to create the Maternity Workforce Strategy – Transforming the Maternity Workforce. This aims to support NHS maternity services deliver more peralised and safer care and improve outcomes for women and their babies by ensuring there is capacity in the workforce nationally.
For more information on the strategy, please visit our Maternity Workforce Transformation Strategy page.
The HEE Maternity Programme is also supporting the implementation of the Neonatal Critical Care Review. For more information on our work supporting neonatal services please visit our Neonatal page.